How long Does Eosinophilic Folliculitis last? The Answer


Eosinophilic folliculitis is a recurrent skin disease most commonly occurring in HIV positive individuals for unknown causes. It may also affect HIV negative individuals with the name of Ofuji disease, which is why the cause for Eosinophillic Folliculitis will determine how long it lasts, although it can vary from several months to several years. It is characterized by itchy red bumps around hair follicles, particularly in upper parts of body, excluding legs and abdomen. If you have recently been diagnosed with eosinophilic folliculitis, then you must be wondering about how long does eosinophilic folliculitis last. Read this oneHOWTO article for more details.
Eosinophilic Folliculitis symptoms
Eosinophilic folliculitis is identified with skin-colored or red bumps (papules) and pustules shaped like dome. The condition looks rather like any other form of folliculitis or acne. The bumps mostly occur on face, neck, trunk and scalp, and can persist for as long as several months. Sometimes, urticarial lesions may also appear, which are larger wheal like patches such as in urticaria. In rare conditions, soles and palms may also develop such pustules and papules. If the condition continues for too long, I may develop into dermatitis or prurigo, probably due to excessive scratching and itching.
Infantile eosinophillic folliculitis
In infants, eosinophillic folliculitis is usually found on the scalp, although they have also reportedly been detected on the child's trunk and extremities in some cases. We should note that cases of infantile easinophillic folliculitis have reportedly been more treatable according to the Division of Pediatrie Dermatology at the Children's Hospital medical Center, Cincinnati, USA[1], as the underlying causes will be different from adults.
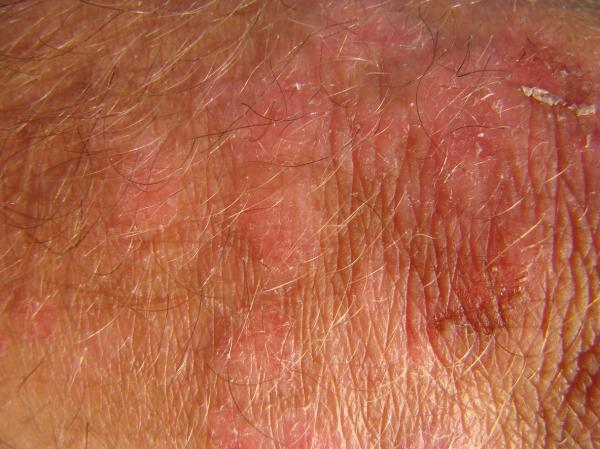
How long does Eosinophillic dermatitis last?
Patients suffering from eosinophilic folliculitis tend to develop sterile papules and pustules recurrently. 50% of the patients develop pruritus, probably with medium intensity. During the entire clinical course of the disease, the patient develops multiple cycles of exacerbating and remitting the symptoms. Depending on individual condition, the skin lesions heal from a few months to as long as several years. The lesions are known to improve with antipsuedomonal treatment procedure, but recur upon therapy cessation.
Eosinophilic Folliculitis causes
Although cytokines, chemotactic factors and intercellular adhesion molecules are associated with the activation of follicular sebaceous units, stimuli that exaggerate these changes are not known so far. Although the exact causes are unknown, it may be significantly linked with immune processes and immunodeficiency, particularly in HIV positive patients. Some theories also point that eosinophils gather around skin follicles in order to attack the sebum.
- The disease may be related to HIV infection and certain lymphomas
- It is also related to a number of drugs like allopurinol, carbamazepine, foscarnet, chemotherapeutic agents, timedium bromide etc.
- Certain infections are also known to cause eosinophilic folliculitis, including hepatitis C virus infection, retrovirus, pityrosporum infection, larva migrans, dermatophyte infection etc.
- The disease is associated with a number of medical conditions as well, including leukemia, atopy, polycythemia vera, myelodysplastic syndrome, sezary syndrome and lymphoma
- It may develop after a solid organ and bone marrow transplantation
- It may be related to the immune dysregulation in some patients
- When it comes to infantile eosinophillic folliculitis, according to D.A Buckley from the department of Dermatology at the Royal Free Hospital in London, UK[2]; this condition can appear in neonates due to erythema toxicum neonatum, and other more rare conditions such as infantile acropustolosis and Leangerhans' cell histiocytosis.
Diagnosis of Eosinophilic Folliculitis
There are different processes to diagnose eosinophilic folliculitis, including:
- Blood test: This test is performed to identify an increase in the normal range of eosinophils in blood, along with an increase in IgE and decrease in IgA and IgG
- Skin biopsy: This test is used to identify eosinophils around the hair follicles
- Clinical symptoms: Clinical diagnosis can be carried out as part of initial assessment of the disease
- CD4 lymphocytes: Patients suffering from HIV infection have low levels of CD4 lymphocytes, which are directly linked with the development of eosinophilic folliculitis

Eosinophilic Folliculitis treatment
Although eosinophilic folliculitis is a recurrent disease and may come back after remittance, there are certain treatment procedures that can help the condition:
- HIV infected individuals may benefit from HAART, short for Highly Active Anti-Retroviral Treatment
- Anti-inflammatory medicines may be prescribed to reduce inflammation
- Antibiotics may be used for secondary bacterial infections
- Oral antihistamines may be indicated if your lesions occur along with severe pruritus
- Topical creams, oral and topical administration of indomethacin and naproxen is recommended to relieve symptoms
- Anti-mite drugs like permethrin are recommended if there are mites in your hair follicles
- Topical treatment with tacrolimus is helpful in suppressing response to immune system
- Phototherapy with UVB and UVA light is shown to give promising results
- Corticosteroids, calcineurin inhibitors, colchicines and retinoids are administered to relieve the condition and prevent it from recurring
- Itraconazole may be prescribed as an anti-fungal medication to control the condition
This article is merely informative, oneHOWTO does not have the authority to prescribe any medical treatments or create a diagnosis. We invite you to visit your doctor if you have any type of condition or pain.
If you want to read similar articles to How long Does Eosinophilic Folliculitis last? The Answer, we recommend you visit our Diseases & secondary effects category.
- http://onlinelibrary.wiley.com/doi/10.1111/j.1525-1470.1984.tb01116.x/full
- http://onlinelibrary.wiley.com/doi/10.1046/j.1365-2230.2001.00807.x/full
- Lucky, Anne W., et al. "Eosinophilic pustular folliculitis in infancy." Pediatric dermatology 1.3 (1984): 202-206.
- Buckley, D. A., S. E. Munn, and E. M. Higgins. "Neonatal eosinophilic pustular folliculitis." Clinical and experimental dermatology 26.3 (2001): 251-255
- .Ellis, Elliot, and Noah Scheinfeld. "Eosinophilic Pustular Folliculitis." American journal of clinical dermatology 5.3 (2004): 189-197.